Improving Opioid-Related Care Through Emergency Medicine–Focused QCDR Measures
The Challenge
Reducing opioid-related harm while meeting emergency medicine quality requirements
The opioid crisis continues to pose a serious public health challenge in the United States. Opioid-involved overdose deaths rose sharply from 49,860 in 2019 to 81,806 in 2022, while prescription opioid-related deaths—though declining—remained significant at 13,026 in 2023. Emergency Departments are often the front door for patients experiencing acute pain, overdose, or opioid withdrawal, placing emergency medicine clinicians at the center of both prevention and intervention.
At the same time, clinicians who bill Medicare are required to participate in the Centers for Medicare & Medicaid Services (CMS) Quality Payment Program (QPP), most commonly through the Merit-based Incentive Payment System (MIPS). For emergency medicine, however, few CMS-developed MIPS quality measures are applicable to day-to-day clinical practice. This creates a gap: clinicians must report quality data, but often lack relevant, actionable measures that meaningfully reflect the care they provide.
The challenge is twofold:
- Improve opioid-related care through evidence-based emergency medicine practices
- Enable clinicians to meet CMS quality reporting requirements using relevant measures
The Solution
Guided by the principle “what gets reviewed, gets improved,” E-CPR has implemented a two-pronged strategy:
As a CMS-approved Qualified Clinical Data Registry (QCDR), Emergency–Clinical Performance Registry (E-CPR) develops targeted quality measures specifically designed for emergency medicine. These measures align national guidelines, public health priorities, and federal reporting requirements—while supporting ongoing quality improvement and financial performance.
1. Promoting appropriate opioid prescribing
To reduce unnecessary opioid exposure and variability in prescribing practices, E-CPR implemented avoidance-focused measures, including:
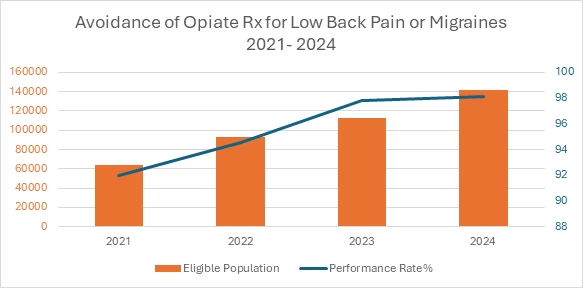
- Avoidance of Opioid Prescriptions for Low Back Pain or Migraines (ECPR46)
Encourages alternative pain management strategies for conditions where narcotic pain medications are not indicated under national guidelines. - Avoidance of Opioids Greater Than Three Days or Long-Acting/Extended-Release Opioids (ECPR55)
Limits the duration and formulation of opioid prescriptions to reduce dependency risk and align prescribing practices with evidence-based standards.
Together, these measures support responsible prescribing decisions at the point of care and reduce the risk of opioid misuse and addiction.
2. Reducing the deadly effects of opioid misuse
Recognizing the need to address overdose risk and support recovery, E-CPR also implemented measures focused on harm reduction and treatment continuity:
- Discharge Prescription of Naloxone After Opioid Poisoning or Overdose (ECPR51)
Ensures patients at risk of overdose have access to life-saving naloxone, addressing national gaps in naloxone distribution. - Opioid Withdrawal: Initiation of Medication-Assisted Treatment (MAT/MOUD) and Referral to Outpatient Treatment (ECPR56)
Facilitates the transition from emergency care to long-term treatment for opioid use disorder, supporting sustained recovery and reducing relapse risk.
The Results
Measurable improvements in patient outcomes and quality performance
Implementation of E-CPR’s opioid-related QCDR measures has led to meaningful, measurable impact:
- Over 411,000 patient lives impacted through responsible opioid prescribing practices
- 21,721 naloxone kits distributed with education since 2021, helping prevent at least 362 opioid overdose deaths
- MAT/MOUD performance rates increased from 55% in 2021 to 67% in 2024, demonstrating improved connection to treatment
- Improved alignment with CMS MIPS requirements, reducing financial risk for participating clinicians
- Up to 9% of Medicare reimbursement protected or enhanced through improved quality performance and avoidance of penalties
By reporting on all patients—not just Medicare beneficiaries—E-CPR provides clinicians with ongoing performance insights that drive sustained improvement over time.
Why It Matters
E-CPR’s QCDR measures demonstrate how specialty-specific quality reporting can improve care, not just compliance. Unlike topped-out CMS measures, these emergency medicine–focused measures identify real gaps in practice, support clinician education, and drive year-over-year improvement.
For clinicians and health systems, this approach delivers both clinical and financial value—improving outcomes for patients while aligning with CMS reimbursement strategies.
Partner with Us
Our QCDR program offers a proven approach that simplifies the reporting process and allows clinicians to focus on patient care.